TMJ massage for jaw clenching and face pain, what it feels like, how many sessions help, and when to skip it
Waking up with a jaw that feels like it’s been working a night shift is common. Clenching can sneak in during sleep, traffic, workouts, even while scrolling. Then the fallout hits: face pain, temple headaches, tooth sensitivity, and that tired “my jaw is heavy” feeling.
TMJ massage can help when the main problem is overworked jaw and neck muscles, not a damaged joint. This article is educational, not a diagnosis. If your symptoms feel intense, new, or confusing, it’s smart to check in with a dentist, doctor, or physical therapist.
Why jaw clenching hurts (and what massage is actually targeting)
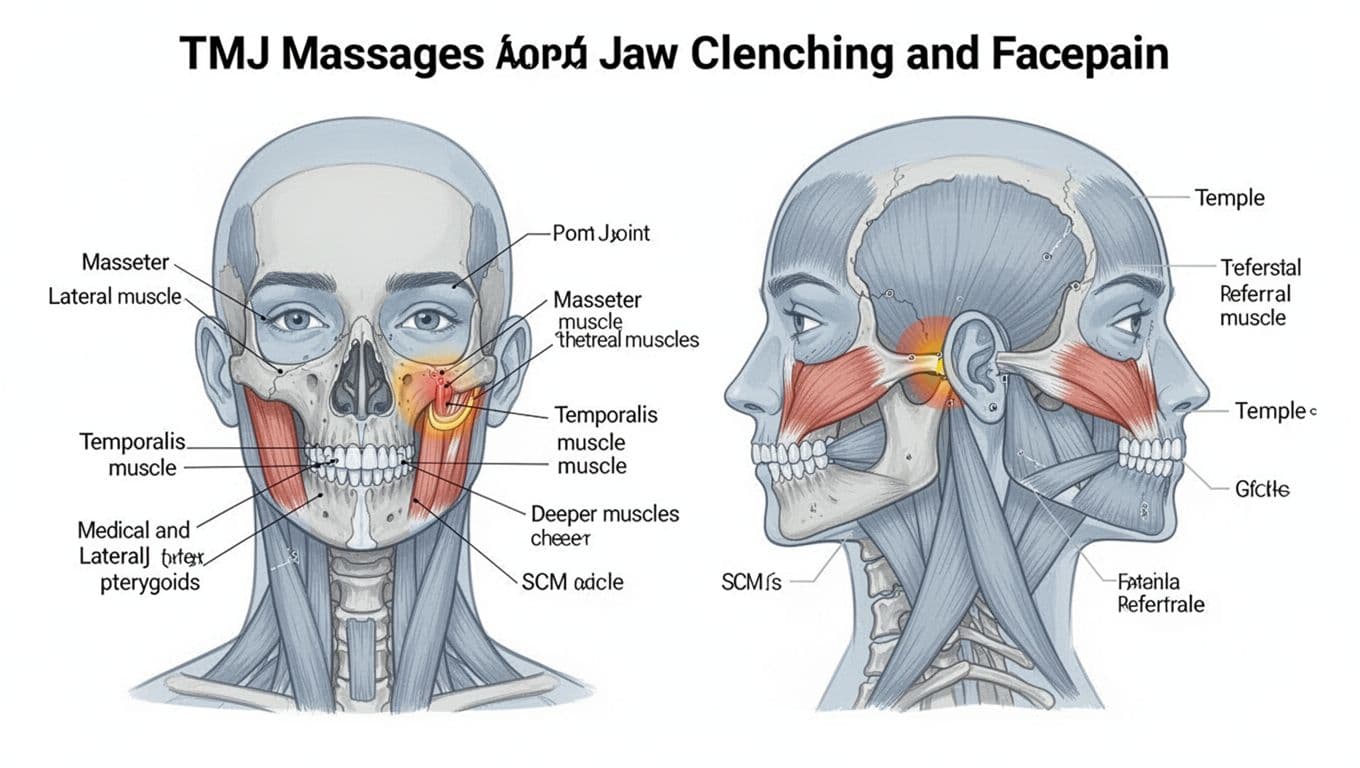 Anatomy map of key jaw muscles and common referral pain patterns, created with AI.
Anatomy map of key jaw muscles and common referral pain patterns, created with AI.
People say “TMJ” when they mean jaw pain, but there are two main buckets:
- Muscle-driven pain (most common): clenching overloads the masseter (cheek), temporalis (temples), and the deeper pterygoids. These muscles can develop tender, ropey spots that refer pain into the cheek, ear area, teeth, temples, and even down the neck.
- Joint-driven symptoms : the TMJ itself can be irritated, inflamed, or not tracking well. That tends to show up as clicking, catching, locking, or bite changes more than broad muscle soreness.
Massage is best at the first bucket. Think of clenching like leaving a parking brake on. The muscles keep firing, blood flow can feel “stuck,” and the nervous system stays on alert. Skilled manual work aims to calm that protective tone, improve circulation, and reduce trigger-point sensitivity.
A key detail: jaw pain is often referred pain , meaning the sore spot is in one place, but your brain feels it somewhere else. A tight masseter can mimic a toothache. A tight temporalis can mimic a headache. For a plain-language overview of temporomandibular disorders and typical symptoms, see the MedlinePlus TMJ disorders summary. For a clinical breakdown of exam findings and when to escalate care, the AAFP rapid evidence review on temporomandibular disorders is a solid reference.
What TMJ massage feels like (pressure, “good hurt,” and normal after-effects)
 Professional jaw massage positioning and gentle contact, created with AI.
Professional jaw massage positioning and gentle contact, created with AI.
A good TMJ-focused session shouldn’t feel like someone trying to “fix” your jaw with force. It’s more like slow, specific pressure that tells your body it’s safe to let go.
Most people notice a mix of these sensations:
- Steady pressure along the cheek (masseter) and temples (temporalis).
- A tender, satisfying “good hurt” that stays tolerable and fades as the therapist holds the spot.
- A referred ache that may travel into the teeth, ear area, eyebrow, or down the neck.
- Warmth and a sense of spreading release, like thawing out a cramped hand.
- Temporary soreness later that day or the next, similar to how you might feel after a deep tissue session on tight shoulders.
Pressure-wise, aim for 2 to 4 out of 10 . That means you can breathe normally and your face stays relaxed. If your body braces, you’re past the helpful zone.
Therapists often work the jaw from the outside (cheeks, temples, under the cheekbone), then connect it to nearby tension patterns in the neck and shoulders (especially the SCM and upper traps). Some providers also use intraoral techniques (gloved work inside the mouth) for deeper pterygoid access, but it should still feel controlled and gentle, never aggressive.
A simple rule: you should leave feeling looser or lighter , even if you’re a bit tender. If you feel more guarded, more locked, or “revved up,” the approach was likely too much, too fast.
If you want a practical overview of massage and simple jaw exercises often paired with it, Cleveland Clinic’s patient-friendly article on TMJ massage and jaw exercises aligns with the gentle, consistency-first approach.
How many sessions help, a simple self-massage plan, and when to skip it
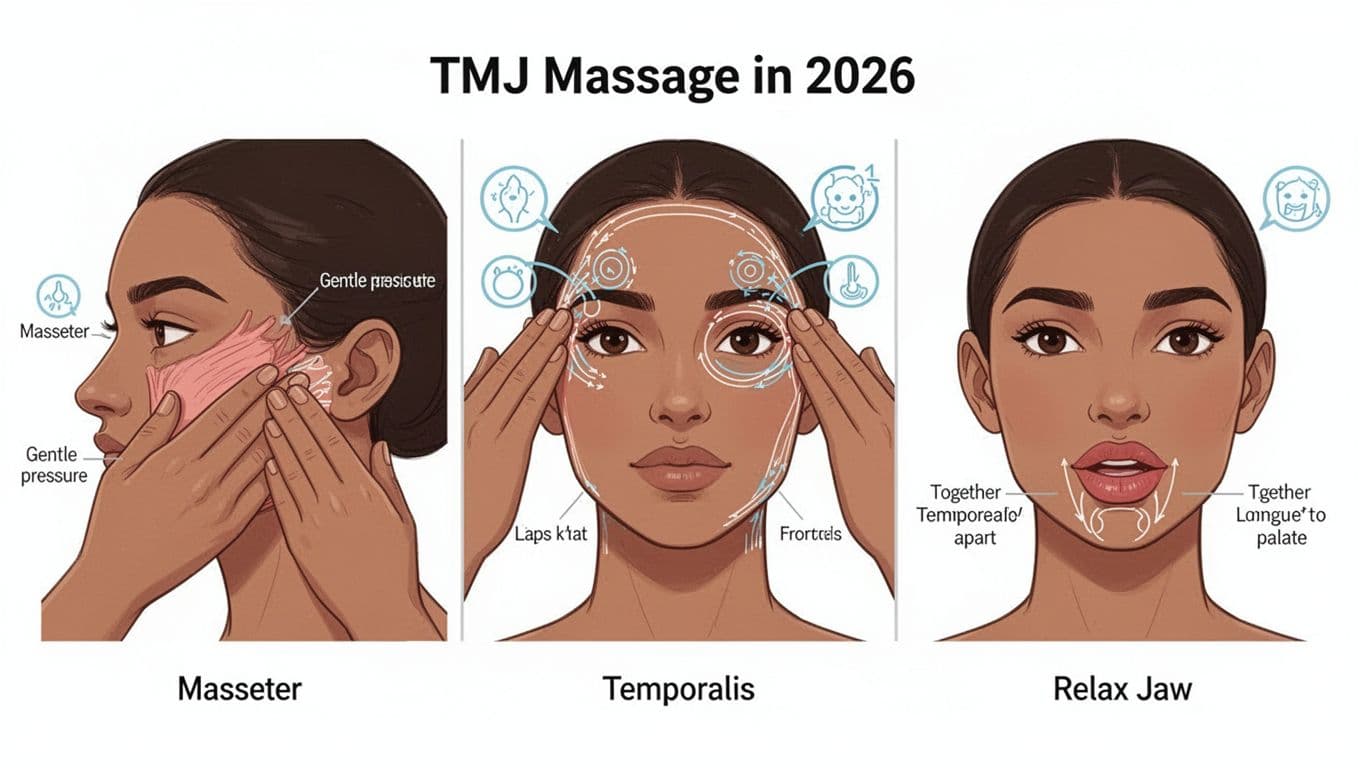 Self-massage hand placement and a relaxed jaw cue, created with AI.
Self-massage hand placement and a relaxed jaw cue, created with AI.
How many sessions usually make a difference?
If your main driver is clenching and muscle tension, a noticeable change often shows up within 2 to 6 sessions . Some people feel a shift after one visit (less temple pressure, easier chewing), but lasting change usually needs repetition.
A realistic timeline looks like this:
- Weeks 1 to 2: focus on calming flare-ups and reducing daily pain.
- Weeks 3 to 6: build consistency, address contributing neck and shoulder tension, and pair with home care.
- Reassess by 4 to 8 weeks: if you’re not improving, it’s time to re-check the diagnosis and plan.
Frequency depends on intensity. Many people do best with professional sessions weekly or every other week at first, plus short home work between appointments.
A simple at-home TMJ massage routine (5 to 8 minutes)
Keep it boring and consistent. Pick 3 to 5 days per week , or daily during a flare if it stays gentle.
- Masseter (cheek): Place two fingers on the thick cheek muscle when you clench. Let the teeth separate, then slowly press and make small circles. Hold tender spots 30 to 90 seconds until the intensity drops.
- Temporalis (temples): Use flat fingers at the temples, slow circles, same 30 to 90 seconds per tender point.
- Jaw “off switch” cue: Lips together, teeth apart , tongue resting on the roof of the mouth. Breathe low and slow for 5 breaths. This helps break the clench habit loop.
If you get sore easily, do less time, less pressure, and more breathing. More force isn’t better.
When to skip TMJ massage (and get checked first)
Massage is not appropriate when there’s a red flag or a condition that needs medical or dental care. Skip massage and get evaluated if you have:
- Recent trauma to the face or jaw, suspected fracture, or suspected dislocation
- Active infection (sinus infection with fever, dental abscess, hot swollen gum, facial cellulitis)
- Uncontrolled bleeding disorders or anticoagulation concerns without medical clearance
- Open wounds, rash, or active skin infection where hands would contact
- Post-surgery on the jaw/face/neck unless your surgeon clears manual work
- Unexplained swelling or a new lump in the jaw, neck, or salivary gland area
- Symptoms that could suggest temporal arteritis (new one-sided temple headache with scalp tenderness, jaw pain with chewing, or vision changes), treat this as urgent
- Known severe osteoporosis of the jaw or other bone-weakening conditions where pressure is risky
Warning sensations that mean “stop”
During self-massage or a session, stop and seek medical or dental advice if you notice:
- Sharp, electric pain
- Numbness or tingling
- Increasing locking , catching, or loss of opening
- Swelling , heat, redness, or fever
- Severe headache that’s new or worsening
- Facial weakness or drooping
- A sudden bite change (teeth don’t meet the same way)
If it’s not just clenching: other tools that often help
Massage works best as part of a plan. If you grind at night or clench under stress, consider pairing manual work with: a dentist-fit night guard when appropriate, heat on the cheeks for 10 minutes, gentle jaw range-of-motion work, posture and neck therapy, and stress or sleep support (some people benefit from CBT-based approaches for bruxism habits).
Conclusion
Jaw clenching pain can feel personal, like your body is “doing it to you,” but it’s often a trainable pattern. TMJ massage usually feels like steady, specific pressure with a tolerable “good hurt,” followed by a looser jaw and less face tension. Many people notice change within 2 to 6 sessions , and it’s worth reassessing if you’re not improving by 4 to 8 weeks . If you’re seeing red flags like swelling, fever, sharp nerve-like pain, facial weakness, or a sudden bite change, skip massage and get evaluated first.
Recent Posts