Massage for Thoracic Outlet Syndrome Arm Tingling: What to Expect
Arm tingling can feel like a bad phone charger, the signal cuts in and out, and you can't trust it. If you've been told you might have thoracic outlet syndrome (TOS), that tingling often isn't random. It's your body saying a nerve, a blood vessel, or both are getting crowded where the neck meets the shoulder.
Massage can help, especially when tight muscles and stiff tissue add pressure in that narrow space. Still, it's normal to wonder what a session will be like, what your therapist will work on, and how quickly symptoms might change.
Here's what to expect from thoracic outlet syndrome massage when arm tingling is part of the picture, plus how to stay safe and get the most from your sessions.
Why thoracic outlet syndrome can cause arm tingling
The "thoracic outlet" is a small passageway between your collarbone and first rib. It's also a busy intersection. Nerves from your neck (the brachial plexus) and major blood vessels travel through it on the way to your arm and hand. When that space gets tight, symptoms can show up fast.
Most people notice tingling in the hand or fingers, aching in the shoulder or neck, or a heavy feeling in the arm. Symptoms often flare with overhead work, long drives, sleeping with arms up, or a slumped desk posture.
A few common "pinch points" show up again and again:
- The scalenes (muscles on the sides of your neck) can tighten and press on nerve pathways.
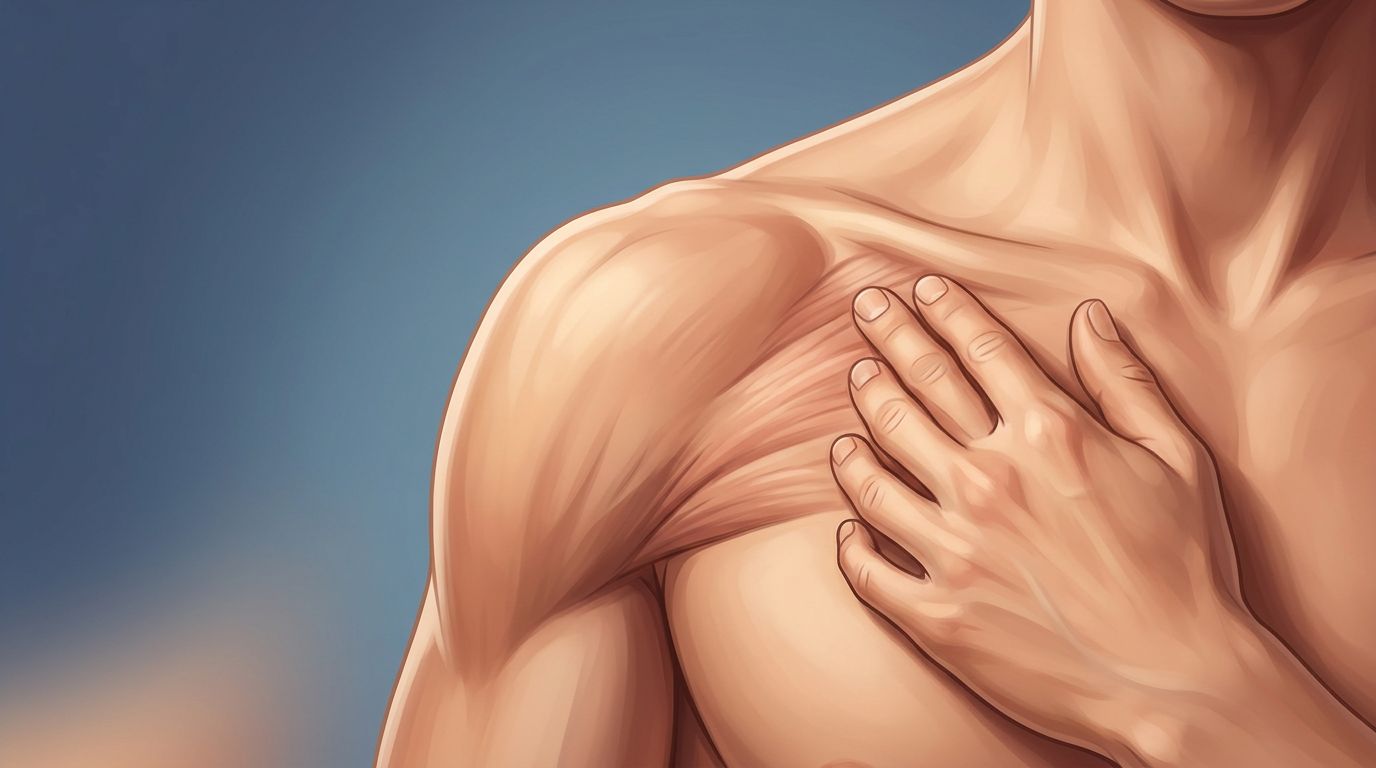
- The pectoralis minor (upper chest) can pull the shoulder forward and narrow space under the collarbone.
- The first rib area and subclavius (under the collarbone) can feel stuck, especially with shallow breathing or rib stiffness.
- The upper traps and levator scapulae (upper back and neck) can stay on guard, which keeps everything tense.
TOS also comes in different forms. Neurogenic TOS (nerve irritation) is the most common. Vascular types involve blood flow changes and need medical attention sooner. That difference matters because massage goals and safety steps change based on your signs.
Thoracic outlet syndrome massage: what it helps, and its limits
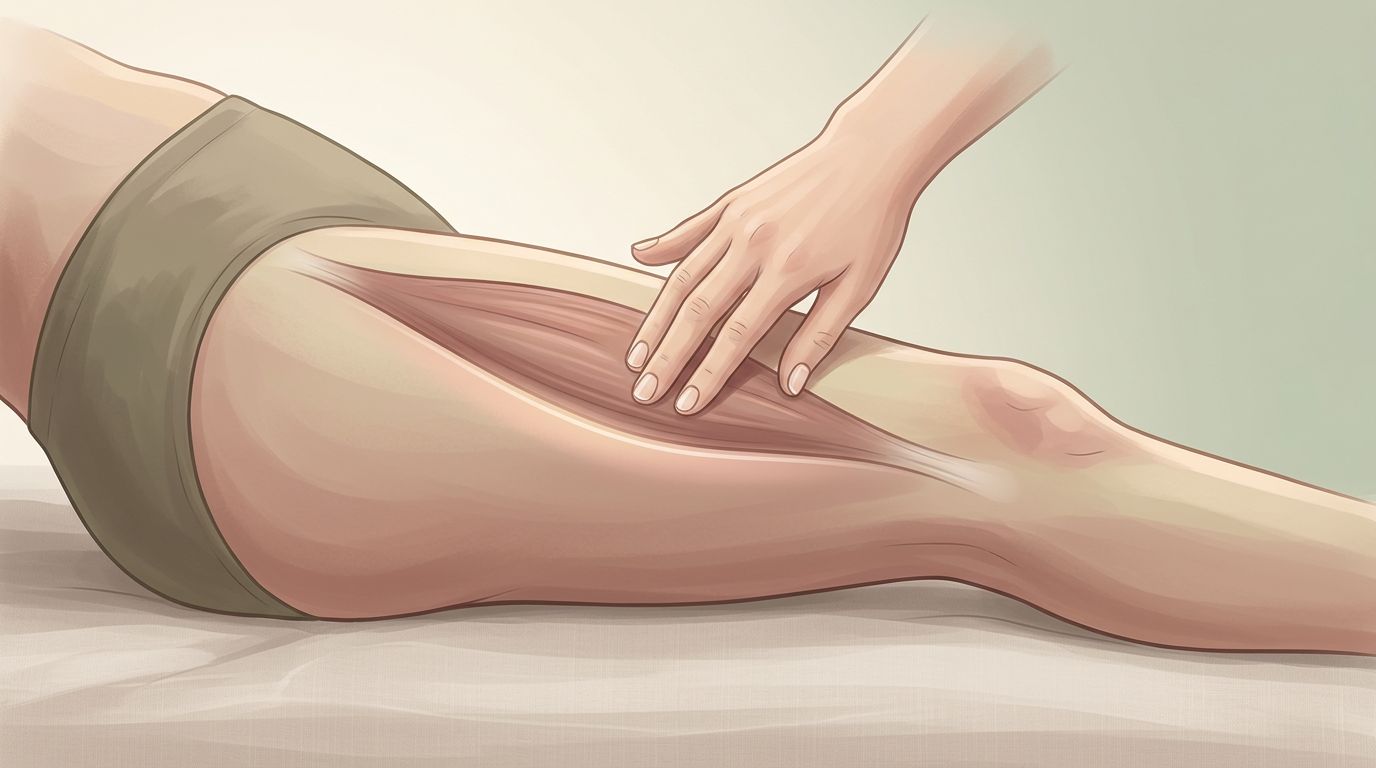
Thoracic outlet syndrome massage usually focuses on reducing the "traffic jam" created by tight muscles, trigger points, and thick fascia around the neck, chest, and shoulder. The aim is to lower tone, improve movement, and give irritated nerves a calmer environment.
In a well-planned session, a therapist may use a mix of:
- Myofascial release to ease restricted tissue in the chest, shoulder front, and upper back.
- Trigger point work (careful, targeted pressure) for knots that refer sensation into the arm.
- Slow deep tissue for pecs, upper traps, and shoulder rotators, as long as your nervous system tolerates it.
- Neck and first-rib focused work that's firm but controlled, not aggressive.
- Breath-led techniques so your rib cage and collarbone area move better.
What massage can't do is "fix" every cause of TOS. If tingling is driven by bone structure, a cervical rib, a recent injury, or true vascular compression, soft tissue work may help symptoms but won't remove the root issue. In that case, massage works best alongside medical care and, often, physical therapy.
A useful rule: massage should calm symptoms over time, not chase them. If every session reproduces strong tingling, the plan needs to change.
What to expect at your appointment (and after you leave)
A good first visit starts with questions, not pressure. Your therapist should ask where the tingling shows up, what triggers it, and what positions help. They may also look at posture, breathing pattern, shoulder position, and neck mobility.
During the session: areas that often matter most
Thoracic outlet syndrome massage is rarely just "neck work." Many people need a full upper-quarter approach. Depending on your comfort and draping, your therapist may spend time on the upper back first, then move to the shoulder and chest, and finish with careful neck work.
Common focus areas include the scalenes, sternocleidomastoid (front neck), pec minor, upper traps, levator scapulae, and the tissues under the collarbone. You might also get gentle work down the arm if the forearm is guarding.
If you're booking a session and want a customizable approach that can prioritize these regions, start by reviewing options for therapeutic massage for pain relief.
How it should feel (and what's a red flag)
Some discomfort is normal, especially when working near sensitive, overworked tissue. Still, the goal is a "good hurt" that eases as you breathe, not a sharp spike that ramps up symptoms.
Here's a quick guide you can keep in mind:
| Sensation during or after | Often OK | Not OK, speak up right away |
|---|---|---|
| Mild tenderness in tight muscles | Yes | No |
| Warmth, loosening, easier neck turn | Yes | No |
| Brief, fading tingling that settles quickly | Sometimes | If it increases or lingers |
| Sharp, electric pain down the arm | No | Yes |
| New weakness, clumsiness, dropping items | No | Yes |
Aftercare: what helps symptoms settle
Plan for your nervous system to "re-calibrate" after bodywork. Many people feel lighter right away, then slightly sore later. That's normal for 24 to 48 hours.
A simple post-massage routine often helps most:
- Hydrate and walk for 10 minutes, movement helps tissues stay calm.
- Use gentle heat on the upper back or chest if you feel guarded (10 to 15 minutes).
- Avoid long overhead tasks that day, give the area a break.
- Try slow breathing with ribs expanding, not shoulders lifting.
Results vary, but many people notice small wins first: less nighttime tingling, fewer flare-ups while driving, or a softer "buzz" in the hand. Lasting change usually takes a few sessions plus posture and strength work between visits.
Get urgent medical care if you notice arm swelling, color change, a cold hand, chest pain, or sudden shortness of breath. Those signs don't belong on a massage table.
Key takeaways and next steps
Arm tingling from TOS can be scary, but it's also often manageable. Thoracic outlet syndrome massage aims to reduce muscle tension and tissue restriction that crowd nerves and vessels near the collarbone and first rib. Expect a session that includes assessment, focused work on neck and chest contributors, and clear feedback about pressure and symptoms.
Your next best step is to track triggers for one week (posture, sleep position, overhead activity) and bring that info to your therapist. With the right plan and steady care, many people feel calmer arms, easier shoulders, and more confidence in day-to-day movement.
Recent Posts